
HIGHLIGHTS OF PRESCRIBING INFORMATION
These highlights do not include all the information needed to use
NASONEX safely and effectively. See full prescribing information
for NASONEX.
NASONEX
®
(mometasone furoate monohydrate) Nasal Spray,
50 mcg
†
†
calculated on the anhydrous basis
Initial U.S. Approval: 1997
--------------------------- RECENT MAJOR CHANGES ---------------------------
Warnings and Precautions
Glaucoma and Cataracts (5.2) 06/2018
----------------------------INDICATIONS AND USAGE ----------------------------
NASONEX is a corticosteroid indicated for:
1. Treatment of Nasal Symptoms of Allergic Rhinitis in patients ≥2
years of age (1.1)
2. Treatment of Nasal Congestion Associated with Seasonal Allergic
Rhinitis in patients ≥2 years of age (1.2)
3. Prophylaxis of Seasonal Allergic Rhinitis in patients ≥12 years of
age (1.3)
4. Treatment of Nasal Polyps in patients ≥18 years of age (1.4)
----------------------- DOSAGE AND ADMINISTRATION -----------------------
For Intranasal Use Only
• Treatment of Nasal Symptoms of Allergic Rhinitis (2.1)
Adults & Adolescents (12 yrs. and older): 2 sprays in each nostril
once daily
Children (2-11 yrs.): 1 spray in each nostril once daily
• Treatment of Nasal Congestion Associated with Seasonal Allergic
Rhinitis (2.2)
Adults & Adolescents (12 yrs. and older): 2 sprays in each nostril
once daily
Children (2-11 yrs.): 1 spray in each nostril once daily
• Prophylaxis of Seasonal Allergic Rhinitis (2.3)
Adults & Adolescents (12 yrs. and older): 2 sprays in each nostril
once daily
• Treatment of Nasal Polyps (2.4)
Adults (18 yrs. and older): 2 sprays in each nostril twice daily. 2
sprays in each nostril once daily may also be effective in some
patients.
--------------------- DOSAGE FORMS AND STRENGTHS ---------------------
Nasal Spray: 50 mcg of mometasone furoate in each 100-microliter
spray (3)
------------------------------- CONTRAINDICATIONS -------------------------------
Patients with known hypersensitivity to mometasone furoate or any of
the ingredients of NASONEX. (4)
----------------------- WARNINGS AND PRECAUTIONS -----------------------
• Epistaxis, nasal ulceration, Candida albicans infection, nasal septal
perforation, impaired wound healing. Monitor patients periodically for
signs of adverse effects on the nasal mucosa. Avoid use in patients
with recent nasal ulcers, nasal surgery, or nasal trauma. (5.1)
• Glaucoma and cataracts. Consider referral to an ophthalmologist in
patients who develop ocular symptoms or use NASONEX long term.
(5.2)
• Potential worsening of existing tuberculosis; fungal, bacterial, viral,
or parasitic infections; or ocular herpes simplex. More serious or
even fatal course of chickenpox or measles in susceptible patients.
Use caution in patients with the above because of the potential for
worsening of these infections. (5.4)
• Hypercorticism and adrenal suppression with higher than
recommended dosages or at the regular dosage in susceptible
individuals. If such changes occur, discontinue NASONEX Nasal
Spray slowly. (5.5)
• Potential reduction in growth velocity in children. Monitor growth
routinely in pediatric patients receiving NASONEX Nasal Spray.
(5.6, 8.4)
------------------------------ ADVERSE REACTIONS ------------------------------
The most common adverse reactions (≥5%) included headache, viral
infection, pharyngitis, epistaxis and cough. (6)
To report SUSPECTED ADVERSE REACTIONS, contact Merck
Sharp & Dohme Corp., a subsidiary of Merck & Co., Inc., at 1-877-
888-4231 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
See 17 for PATIENT COUNSELING INFORMATION and FDA-
approved patient labeling.
Revised: 06/2018
FULL PRESCRIBING INFORMATION: CONTENTS*
1 INDICATIONS AND USAGE
1.1
Treatment of Allergic Rhinitis
1.2 Treatment of Nasal Congestion Associated with Seasonal
Allergic Rhinitis
1.3 Prophylaxis of Seasonal Allergic Rhinitis
1.4 Treatment of Nasal Polyps
2 DOSAGE AND ADMINISTRATION
2.1 Treatment of Allergic Rhinitis
2.2 Treatment of Nasal Congestion Associated with Seasonal
Allergic Rhinitis
2.3 Prophylaxis of Seasonal Allergic Rhinitis
2.4 Treatment of Nasal Polyps
3 DOSAGE FORMS AND STRENGTHS
4 CONTRAINDICATIONS
5 WARNINGS AND PRECAUTIONS
5.1 Local Nasal Effects
5.2 Glaucoma and Cataracts
5.3 Hypersensitivity Reactions
5.4 Immunosuppression
5.5 Hypothalamic-Pituitary-Adrenal Axis Effect
5.6 Effect on Growth
6 ADVERSE REACTIONS
6.1 Clinical Trials Experience
6.2 Post-Marketing Experience
7 DRUG INTERACTIONS
8 USE IN SPECIFIC POPULATIONS
8.1 Pregnancy
8.3 Nursing Mothers
8.4 Pediatric Use
8.5 Geriatric Use
8.6 Hepatic Impairment
10 OVERDOSAGE
11 DESCRIPTION
12 CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
12.2 Pharmacodynamics
12.3 Pharmacokinetics
13 NONCLINICAL TOXICOLOGY
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
13.2 Animal Toxicology and/or Pharmacology
14 CLINICAL STUDIES
14.1 Allergic Rhinitis in Adults and Adolescents
14.2 Allergic Rhinitis in Pediatrics
14.3 Nasal Polyps in Adults 18 Years of Age and Older
14.4 Nasal Congestion Associated with Seasonal Allergic
Rhinitis
16 HOW SUPPLIED/STORAGE AND HANDLING
17 PATIENT COUNSELING INFORMATION
17.1 Local Nasal Effect
17.2 Glaucoma and Cataracts
17.3 Immunosuppression
17.4 Use Regularly for Best Effect
* Sections or subsections omitted from the full prescribing information
are not listed.
Reference ID: 4281761
This label may not be the latest approved by FDA.
For current labeling information, please visit https://www.fda.gov/drugsatfda

2
FULL PRESCRIBING INFORMATION
1 INDICATIONS AND USAGE
1.1 Treatment of Allergic Rhinitis
NASONEX
®
Nasal Spray 50 mcg is indicated for the treatment of the nasal symptoms of seasonal allergic and perennial allergic rhinitis, in adults
and pediatric patients 2 years of age and older.
1.2 Treatment of Nasal Congestion Associated with Seasonal Allergic Rhinitis
NASONEX Nasal Spray 50 mcg is indicated for the relief of nasal congestion associated with seasonal allergic rhinitis, in adults and pediatric
patients 2 years of age and older.
1.3 Prophylaxis of Seasonal Allergic Rhinitis
NASONEX Nasal Spray 50 mcg is indicated for the prophylaxis of the nasal symptoms of seasonal allergic rhinitis in adult and adolescent
patients 12 years and older.
1.4 Treatment of Nasal Polyps
NASONEX Nasal Spray 50 mcg is indicated for the treatment of nasal polyps in patients 18 years of age and older.
2 DOSAGE AND ADMINISTRATION
Administer NASONEX Nasal Spray 50 mcg by the intranasal route only. Prior to initial use of NASONEX Nasal Spray, 50 mcg, the pump must be
primed by actuating ten times or until a fine spray appears. The pump may be stored unused for up to 1 week without repriming. If unused for more than
1 week, reprime by actuating two times, or until a fine spray appears.
2.1 Treatment of Allergic Rhinitis
Adults and Adolescents 12 Years of Age and Older:
The recommended dose for treatment of the nasal symptoms of seasonal allergic and perennial allergic rhinitis is 2 sprays (50 mcg of
mometasone furoate in each spray) in each nostril once daily (total daily dose of 200 mcg).
Children 2 to 11 Years of Age:
The recommended dose for treatment of the nasal symptoms of seasonal allergic and perennial allergic rhinitis is 1 spray (50 mcg of
mometasone furoate in each spray) in each nostril once daily (total daily dose of 100 mcg).
2.2 Treatment of Nasal Congestion Associated with Seasonal Allergic Rhinitis
Adults and Adolescents 12 Years of Age and Older:
The recommended dose for treatment of nasal congestion associated with seasonal allergic rhinitis is two sprays (50 mcg of mometasone
furoate in each spray) in each nostril once daily (total daily dose of 200 mcg).
Children 2 to 11 Years of Age:
The recommended dose for treatment of nasal congestion associated with seasonal allergic rhinitis is one spray (50 mcg of mometasone furoate
in each spray) in each nostril once daily (total daily dose of 100 mcg).
2.3 Prophylaxis of Seasonal Allergic Rhinitis
Adults and Adolescents 12 Years of Age and Older:
The recommended dose for prophylaxis treatment of nasal symptoms of seasonal allergic rhinitis is 2 sprays (50 mcg of mometasone furoate in
each spray) in each nostril once daily (total daily dose of 200 mcg).
In patients with a known seasonal allergen that precipitates nasal symptoms of seasonal allergic rhinitis, prophylaxis with NASONEX Nasal
Spray 50 mcg (200 mcg/day) is recommended 2 to 4 weeks prior to the anticipated start of the pollen season.
2.4 Treatment of Nasal Polyps
Adults 18 Years of Age and Older:
The recommended dose for the treatment of nasal polyps is 2 sprays (50 mcg of mometasone furoate in each spray) in each nostril twice daily
(total daily dose of 400 mcg). A dose of 2 sprays (50 mcg of mometasone furoate in each spray) in each nostril once daily (total daily dose of 200 mcg) is
also effective in some patients.
3 DOSAGE FORMS AND STRENGTHS
NASONEX Nasal Spray 50 mcg is a metered-dose, manual pump spray unit containing an aqueous suspension of mometasone furoate
monohydrate equivalent to 0.05% w/w mometasone furoate calculated on the anhydrous basis.
After initial priming (10 actuations), each actuation of the pump delivers a metered spray containing 100 mg or 100 microliter of suspension
containing mometasone furoate monohydrate equivalent to 50 mcg of mometasone furoate calculated on the anhydrous basis. Each bottle of NASONEX
Nasal Spray 50 mcg provides 120 sprays.
4 CONTRAINDICATIONS
NASONEX Nasal Spray is contraindicated in patients with known hypersensitivity to mometasone furoate or any of its ingredients.
Reference ID: 4281761
This label may not be the latest approved by FDA.
For current labeling information, please visit https://www.fda.gov/drugsatfda

3
5 WARNINGS AND PRECAUTIONS
5.1 Local Nasal Effects
Epistaxis
In clinical studies, epistaxis was observed more frequently in patients with allergic rhinitis with NASONEX Nasal Spray than those who received
placebo [see Adverse Reactions (6)].
Candida Infection
In clinical studies with NASONEX Nasal Spray 50 mcg, the development of localized infections of the nose and pharynx with Candida albicans
has occurred. When such an infection develops, use of NASONEX Nasal Spray 50 mcg should be discontinued and appropriate local or systemic
therapy instituted, if needed.
Nasal Septum Perforation
Instances of nasal septum perforation have been reported following the intranasal application of corticosteroids. As with any long-term topical
treatment of the nasal cavity, patients using NASONEX Nasal Spray 50 mcg over several months or longer should be examined periodically for possible
changes in the nasal mucosa.
Impaired Wound Healing
Because of the inhibitory effect of corticosteroids on wound healing, patients who have experienced recent nasal septum ulcers, nasal surgery,
or nasal trauma should not use a nasal corticosteroid until healing has occurred.
5.2 Glaucoma and Cataracts
Glaucoma and cataracts may be reported with systemic and topical (including intranasal, inhaled and intraocular) corticosteroid use. Consider
referral to an ophthalmologist in patients who develop ocular symptoms or use NASONEX long term [see Adverse Reactions (6)].
Glaucoma and cataract formation was evaluated in one controlled study of 12 weeks’ duration and one uncontrolled study of 12 months’ duration
in patients treated with NASONEX Nasal Spray, 50 mcg at 200 mcg/day, using intraocular pressure measurements and slit lamp examination. No
significant change from baseline was noted in the mean intraocular pressure measurements for the 141 NASONEX-treated patients in the 12-week
study, as compared with 141 placebo-treated patients. No individual NASONEX-treated patient was noted to have developed a significant elevation in
intraocular pressure or cataracts in this 12-week study. Likewise, no significant change from baseline was noted in the mean intraocular pressure
measurements for the 139 NASONEX-treated patients in the 12-month study and again, no cataracts were detected in these patients. Nonetheless,
intranasal and inhaled corticosteroids have been associated with the development of glaucoma and/or cataracts.
5.3 Hypersensitivity Reactions
Hypersensitivity reactions including instances of wheezing may occur after the intranasal administration of mometasone furoate monohydrate.
Discontinue NASONEX Nasal Spray if such reactions occur [see Contraindications (4)].
5.4 Immunosuppression
Persons who are on drugs which suppress the immune system are more susceptible to infections than healthy individuals. Chickenpox and
measles, for example, can have a more serious or even fatal course in nonimmune children or adults on corticosteroids. In such children or adults who
have not had these diseases, particular care should be taken to avoid exposure. How the dose, route, and duration of corticosteroid administration affect
the risk of developing a disseminated infection is not known. The contribution of the underlying disease and/or prior corticosteroid treatment to the risk is
also not known. If exposed to chickenpox, prophylaxis with varicella zoster immune globulin (VZIG) may be indicated. If exposed to measles, prophylaxis
with pooled intramuscular immunoglobulin (IG) may be indicated. (See the respective package inserts for complete VZIG and IG prescribing
information.) If chickenpox develops, treatment with antiviral agents may be considered.
Corticosteroids should be used with caution, if at all, in patients with active or quiescent tuberculous infection of the respiratory tract, or in
untreated fungal, bacterial, systemic viral infections, or ocular herpes simplex because of the potential for worsening of these infections.
5.5 Hypothalamic-Pituitary-Adrenal Axis Effect
Hypercorticism and Adrenal Suppression
When intranasal steroids are used at higher than recommended dosages or in susceptible individuals at recommended dosages, systemic
corticosteroid effects such as hypercorticism and adrenal suppression may appear. If such changes occur, the dosage of NASONEX Nasal Spray should
be discontinued slowly, consistent with accepted procedures for discontinuing oral corticosteroid therapy.
5.6 Effect on Growth
Corticosteroids may cause a reduction in growth velocity when administered to pediatric patients. Monitor the growth routinely of pediatric
patients receiving NASONEX Nasal Spray. To minimize the systemic effects of intranasal corticosteroids, including NASONEX Nasal Spray, titrate each
patient’s dose to the lowest dosage that effectively controls his/her symptoms [see Use in Specific Populations (8.4)].
6 ADVERSE REACTIONS
Systemic and local corticosteroid use may result in the following:
• Epistaxis, ulcerations, Candida albicans infection, impaired wound healing [see Warnings and Precautions (5.1)]
• Glaucoma and cataracts [see Warnings and Precautions (5.2)]
• Immunosuppression [see Warnings and Precautions (5.4)]
• Hypothalamic-pituitary-adrenal (HPA) axis effects, including growth reduction [see Warnings and Precautions (5.5, 5.6), Use in Specific
Populations (8.4)]
Reference ID: 4281761
This label may not be the latest approved by FDA.
For current labeling information, please visit https://www.fda.gov/drugsatfda

4
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be
directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
Allergic Rhinitis
Adults and adolescents 12 years of age and older
In controlled US and international clinical studies, a total of 3210 adult and adolescent patients 12 years and older with allergic rhinitis received
treatment with NASONEX Nasal Spray 50 mcg at doses of 50 to 800 mcg/day. The majority of patients (n=2103) were treated with 200 mcg/day. A total
of 350 adult and adolescent patients have been treated for one year or longer. Adverse events did not differ significantly based on age, sex, or race.
Four percent or less of patients in clinical trials discontinued treatment because of adverse events and the discontinuation rate was similar for the vehicle
and active comparators.
All adverse events (regardless of relationship to treatment) reported by 5% or more of adult and adolescent patients ages 12 years and older
who received NASONEX Nasal Spray 50 mcg, 200 mcg/day vs. placebo and that were more common with NASONEX Nasal Spray 50 mcg than
placebo, are displayed in TABLE 1 below.
TABLE 1: ADULT AND ADOLESCENT PATIENTS 12 YEARS AND OLDER – ADVERSE EVENTS FROM CONTROLLED CLINICAL TRIALS IN
SEASONAL ALLERGIC AND PERENNIAL ALLERGIC RHINITIS (PERCENT OF PATIENTS REPORTING)
NASONEX
200 mcg
(n=2103)
VEHICLE
PLACEBO
(n=1671)
Headache
26
22
Viral Infection
14
11
Pharyngitis
12
10
Epistaxis/Blood-Tinged
Mucus
11
6
Coughing
7
6
Upper Respiratory Tract
Infection
6
2
Dysmenorrhea
5
3
Musculoskeletal Pain
5
3
Sinusitis
5
3
Other adverse events which occurred in less than 5% but greater than or equal to 2% of adult and adolescent patients (ages 12 years and older)
treated with NASONEX Nasal Spray 50 mcg, 200-mcg/day (regardless of relationship to treatment), and more frequently than in the placebo group
included: arthralgia, asthma, bronchitis, chest pain, conjunctivitis, diarrhea, dyspepsia, earache, flu-like symptoms, myalgia, nausea, and rhinitis.
Pediatric patients <12 years of age
In controlled US and international studies, a total of 990 pediatric patients (ages 3 to 11 years) with allergic rhinitis received treatment with
NASONEX Nasal Spray 50 mcg, at doses of 25 to 200 mcg/day. The majority of pediatric patients (n=720) were treated with 100 mcg/day. A total of 163
pediatric patients have been treated for one year or longer. Two percent or less of patients in clinical trials who received NASONEX Nasal Spray 50 mcg
discontinued treatment because of adverse events and the discontinuation rate was similar for the placebo and active comparators.
Adverse events which occurred in ≥5% of pediatric patients (ages 3 to 11 years) treated with NASONEX Nasal Spray 50 mcg, 100 mcg/day vs.
placebo (regardless of relationship to treatment) and more frequently than in the placebo group included upper respiratory tract infection (5% in
NASONEX Nasal Spray 50 mcg group vs. 4% in placebo) and vomiting (5% in NASONEX Nasal Spray 50 mcg group vs. 4% in placebo).
Other adverse events which occurred in less than 5% but greater than or equal to 2% of pediatric patients (ages 3 to 11 years) treated with
NASONEX Nasal Spray 50 mcg, 100 mcg/day vs. placebo (regardless of relationship to treatment) and more frequently than in the placebo group
included: diarrhea, nasal irritation, otitis media, and wheezing.
The adverse event (regardless of relationship to treatment) reported by 5% of pediatric patients ages 2 to 5 years who received NASONEX
Nasal Spray, 50 mcg, 100 mcg/day in a clinical trial vs. placebo including 56 subjects (28 each NASONEX Nasal Spray, 50 mcg and placebo) and that
was more common with NASONEX Nasal Spray, 50 mcg than placebo, included: upper respiratory tract infection (7% vs. 0%, respectively). The other
adverse event which occurred in less than 5% but greater than or equal to 2% of mometasone furoate pediatric patients ages 2 to 5 years treated with
100 mcg doses vs. placebo (regardless of relationship to treatment) and more frequently than in the placebo group included: skin trauma.
Nasal Polyps
Adults 18 years of age and older
In controlled clinical studies, the types of adverse events observed in patients with nasal polyps were similar to those observed for patients with
allergic rhinitis. A total of 594 adult patients (ages 18 to 86 years) received NASONEX Nasal Spray 50 mcg at doses of 200 mcg once or twice daily for
up to 4 months for treatment of nasal polyps. The overall incidence of adverse events for patients treated with NASONEX Nasal Spray 50 mcg was
Reference ID: 4281761
This label may not be the latest approved by FDA.
For current labeling information, please visit https://www.fda.gov/drugsatfda
5
comparable to patients with the placebo except for epistaxis, which was 9% for 200 mcg once daily, 13% for 200 mcg twice daily, and 5% for the
placebo.
Nasal ulcers and nasal and oral candidiasis were also reported in patients treated with NASONEX Nasal Spray 50 mcg primarily in patients
treated for longer than 4 weeks.
Nasal Congestion Associated with Seasonal Allergic Rhinitis
A total of 1008 patients aged 12 years and older received NASONEX Nasal Spray 50 mcg 200 mcg/day (n=506) or placebo (n=502) for 15 days.
Adverse events that occurred more frequently in patients treated with NASONEX Nasal Spray 50 mcg than in patients with the placebo included sinus
headache (1.2% in NASONEX Nasal Spray 50 mcg group vs. 0.2% in placebo) and epistaxis (1% in NASONEX Nasal Spray 50 mcg group vs. 0.2% in
placebo) and the overall adverse event profile was similar to that observed in the other allergic rhinitis trials.
6.2 Post-Marketing Experience
The following adverse reactions have been identified during the post-marketing period for NASONEX Nasal Spray 50 mcg: nasal burning and
irritation, anaphylaxis and angioedema, disturbances in taste and smell, nasal septal perforation, and vision blurred. Because these reactions are
reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to
drug exposure.
7 DRUG INTERACTIONS
No formal drug-drug interaction studies have been conducted with NASONEX Nasal Spray 50 mcg.
Inhibitors of Cytochrome P450 3A4: Studies have shown that mometasone furoate is primarily and extensively metabolized in the liver of all
species investigated and undergoes extensive metabolism to multiple metabolites. In vitro studies have confirmed the primary role of cytochrome
CYP3A4 in the metabolism of this compound.
Concomitant administration of CYP3A4 inhibitors may inhibit the metabolism of, and increase the systemic exposure to, mometasone furoate
and potentially increase the risk for systemic corticosteroid side effects. Caution should be exercised when considering the coadministration of
NASONEX Nasal Spray 50 mcg with long-term ketoconazole and other known strong CYP3A4 inhibitors (e.g., ritonavir, cobicistat-containing products,
atazanavir, clarithromycin, indinavir, itraconazole, nefazodone, nelfinavir, saquinavir, telithromycin) [see Clinical Pharmacology (12.3)]. Consider the
benefit of coadministration versus the potential risk of systemic corticosteroid effects, in which case patients should be monitored for systemic
corticosteroid side effects.
8 USE IN SPECIFIC POPULATIONS
8.1 Pregnancy
Teratogenic Effects: Pregnancy Category C: There are no adequate and well-controlled studies in pregnant women. NASONEX Nasal Spray
50 mcg, like other corticosteroids, should be used during pregnancy only if the potential benefits justify the potential risk to the fetus. Experience with
oral corticosteroids since their introduction in pharmacologic, as opposed to physiologic, doses suggests that rodents are more prone to teratogenic
effects from corticosteroids than humans. In addition, because there is a natural increase in corticosteroid production during pregnancy, most women will
require a lower exogenous corticosteroid dose and many will not need corticosteroid treatment during pregnancy.
In mice, mometasone furoate caused cleft palate at subcutaneous doses (less than the MRDID in adults on a mcg/m
2
basis). Fetal survival was
reduced at approximately 2 times the MRDID in adults on a mcg/m
2
basis. No toxicity was observed at less than the MRDID in adults on a mcg/m
2
basis.
In rats, mometasone furoate produced umbilical hernia at topical dermal doses approximately 10 times the MRDID in adults on a mcg/m
2
basis.
A topical dermal dose approximately 6 times the MRDID in adults on a mcg/m
2
basis produced delays in ossification, but no malformations.
In rabbits, mometasone furoate caused multiple malformations (e.g., flexed front paws, gallbladder agenesis, umbilical hernia, and hydrocephaly)
at topical dermal doses approximately 6 times the MRDID in adults on a mcg/m
2
basis. In an oral study, mometasone furoate increased resorptions and
caused cleft palate and/or head malformations (hydrocephaly or domed head) at approximately 30 times the MRDID in adults on a mcg/m
2
basis. At
approximately 110 times the MRDID in adults on a mcg/m
2
basis, most litters were aborted or resorbed. No toxicity was observed at approximately 6
times the MRDID in adults on a mcg/m
2
basis.
When rats received subcutaneous doses of mometasone furoate throughout pregnancy or during the later stages of pregnancy, a dose less than
the MRDID in adults on a mcg/m
2
basis caused prolonged and difficult labor and reduced the number of live births, birth weight, and early pup survival.
Nonteratogenic Effects: Hypoadrenalism may occur in infants born to women receiving corticosteroids during pregnancy. Such infants should
be carefully monitored.
8.3 Nursing Mothers
It is not known if mometasone furoate is excreted in human milk. Because other corticosteroids are excreted in human milk, caution should be
used when NASONEX Nasal Spray, 50 mcg is administered to nursing women.
8.4 Pediatric Use
The safety and effectiveness of NASONEX Nasal Spray 50 mcg for allergic rhinitis in children 12 years of age and older have been established
[see Adverse Reactions (6.1) and Clinical Studies (14.1)]. Use of NASONEX Nasal Spray 50 mcg for allergic rhinitis in pediatric patients 2 to 11 years of
age is supported by safety and efficacy data from clinical studies. Seven hundred and twenty (720) patients 3 to 11 years of age with allergic rhinitis
were treated with mometasone furoate nasal spray 50 mcg (100 mcg total daily dose) in controlled clinical trials [see Adverse Reactions (6.1) and
Clinical Studies (14.2)]. Twenty-eight (28) patients 2 to 5 years of age with allergic rhinitis were treated with mometasone furoate nasal spray 50 mcg
(100 mcg total daily dose) in a controlled trial to evaluate safety [see Adverse Reactions (6.1)]. Safety and effectiveness of NASONEX Nasal Spray 50
mcg for allergic rhinitis in children less than 2 years of age have not been established.
Reference ID: 4281761
This label may not be the latest approved by FDA.
For current labeling information, please visit https://www.fda.gov/drugsatfda
6
The safety and effectiveness of NASONEX Nasal Spray for the treatment of nasal polyps in children less than 18 years of age have not been
established. One 4-month trial was conducted to evaluate the safety and efficacy of NASONEX in the treatment of nasal polyps in pediatric patients 6 to
17 years of age. The primary objective of the study was to evaluate safety; efficacy parameters were collected as secondary endpoints. A total of 127
patients with nasal polyps were randomized to placebo or NASONEX Nasal Spray 100 mcg once or twice daily (patients 6 to 11 years of age) or 200
mcg once or twice daily (patients 12 to 17 years of age). The results of this trial did not support the efficacy of NASONEX Nasal Spray in the treatment of
nasal polyps in pediatric patients. The adverse events reported in this trial were similar to the adverse events reported in patients 18 years of age and
older with nasal polyps.
Controlled clinical studies have shown intranasal corticosteroids may cause a reduction in growth velocity in pediatric patients. This effect has
been observed in the absence of laboratory evidence of hypothalamic-pituitary-adrenal (HPA) axis suppression, suggesting that growth velocity is a
more sensitive indicator of systemic corticosteroid exposure in pediatric patients than some commonly used tests of HPA axis function. The long-term
effects of this reduction in growth velocity associated with intranasal corticosteroids, including the impact on final adult height, are unknown. The
potential for “catch up” growth following discontinuation of treatment with intranasal corticosteroids has not been adequately studied. The growth of
pediatric patients receiving intranasal corticosteroids, including NASONEX Nasal Spray, 50 mcg, should be monitored routinely (e.g., via stadiometry).
The potential growth effects of prolonged treatment should be weighed against clinical benefits obtained and the availability of safe and effective
noncorticosteroid treatment alternatives. To minimize the systemic effects of intranasal corticosteroids, including NASONEX Nasal Spray, 50 mcg, each
patient should be titrated to his/her lowest effective dose.
A clinical study to assess the effect of NASONEX Nasal Spray 50 mcg (100 mcg total daily dose) on growth velocity has been conducted in
pediatric patients 3 to 9 years of age with allergic rhinitis. No statistically significant effect on growth velocity was observed for NASONEX Nasal Spray
50 mcg compared to placebo following one year of treatment. No evidence of clinically relevant HPA axis suppression was observed following a 30-
minute cosyntropin infusion.
The potential of NASONEX Nasal Spray 50 mcg to cause growth suppression in susceptible patients or when given at higher doses cannot be
ruled out.
8.5 Geriatric Use
A total of 280 patients above 64 years of age with allergic rhinitis or nasal polyps (age range 64 to 86 years) have been treated with NASONEX
Nasal Spray 50 mcg for up to 3 or 4 months, respectively. The adverse reactions reported in this population were similar in type and incidence to those
reported by younger patients.
8.6 Hepatic Impairment
Concentrations of mometasone furoate appear to increase with severity of hepatic impairment [see Clinical Pharmacology (12.3)].
10 OVERDOSAGE
There are no data available on the effects of acute or chronic overdosage with NASONEX Nasal Spray 50 mcg. Because of low systemic
bioavailability, and an absence of acute drug-related systemic findings in clinical studies, overdose is unlikely to require any therapy other than
observation. Intranasal administration of 1600 mcg (4 times the recommended dose of NASONEX Nasal Spray 50 mcg for the treatment of nasal polyps
in patients 18 years of age and older) daily for 29 days, to healthy human volunteers, showed no increased incidence of adverse events. Single
intranasal doses up to 4000 mcg and oral inhalation doses up to 8000 mcg have been studied in human volunteers with no adverse effects reported.
Chronic over dosage with any corticosteroid may result in signs or symptoms of hypercorticism [see Warnings and Precautions (5.5)]. Acute overdosage
with this dosage form is unlikely since one bottle of NASONEX Nasal Spray 50 mcg contains approximately 8500 mcg of mometasone furoate.
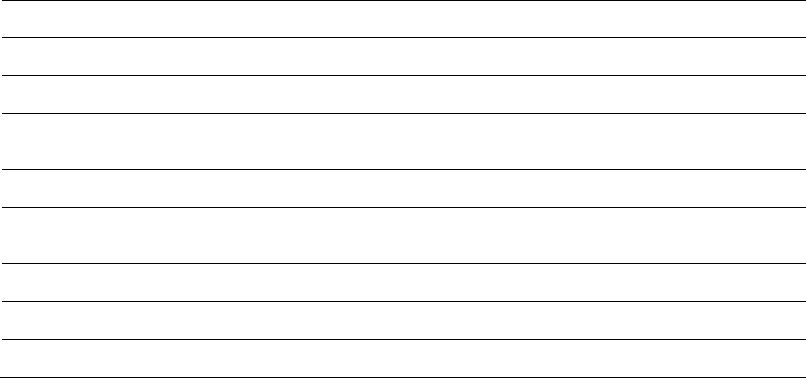
11 DESCRIPTION
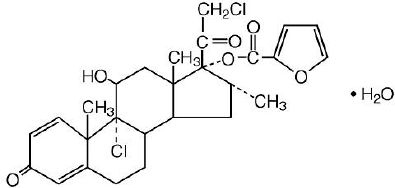
Mometasone furoate monohydrate, the active component of NASONEX Nasal Spray, 50 mcg, is an anti-inflammatory corticosteroid having the
chemical name, 9,21-Dichloro-11ß,17-dihydroxy-16α-methylpregna-1,4-diene-3,20-dione17-(2 furoate) monohydrate, and the following chemical
structure:
Mometasone furoate monohydrate is a white powder, with an empirical formula of C
27
H
30
C
l2
O
6
•H
2
O, and a molecular weight of 539.45. It is
practically insoluble in water; slightly soluble in methanol, ethanol, and isopropanol; soluble in acetone and chloroform; and freely soluble in
tetrahydrofuran. Its partition coefficient between octanol and water is greater than 5000.
NASONEX Nasal Spray 50 mcg is a metered-dose, manual pump spray unit containing an aqueous suspension of mometasone furoate
monohydrate equivalent to 0.05% w/w mometasone furoate calculated on the anhydrous basis; in an aqueous medium containing glycerin,
microcrystalline cellulose and carboxymethylcellulose sodium, sodium citrate, citric acid, benzalkonium chloride, and polysorbate 80. The pH is between
4.3 and 4.9.
Reference ID: 4281761
This label may not be the latest approved by FDA.
For current labeling information, please visit https://www.fda.gov/drugsatfda
7
12 CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
NASONEX Nasal Spray 50 mcg is a corticosteroid demonstrating potent anti-inflammatory properties. The precise mechanism of corticosteroid
action on allergic rhinitis is not known. Corticosteroids have been shown to have a wide range of effects on multiple cell types (e.g., mast cells,
eosinophils, neutrophils, macrophages, and lymphocytes) and mediators (e.g., histamine, eicosanoids, leukotrienes, and cytokines) involved in
inflammation.
In two clinical studies utilizing nasal antigen challenge, NASONEX Nasal Spray, 50 mcg decreased some markers of the early- and late-phase
allergic response. These observations included decreases (vs. placebo) in histamine and eosinophil cationic protein levels, and reductions (vs. baseline)
in eosinophils, neutrophils, and epithelial cell adhesion proteins. The clinical significance of these findings is not known.
The effect of NASONEX Nasal Spray, 50 mcg on nasal mucosa following 12 months of treatment was examined in 46 patients with allergic
rhinitis. There was no evidence of atrophy and there was a marked reduction in intraepithelial eosinophilia and inflammatory cell infiltration (e.g.,
eosinophils, lymphocytes, monocytes, neutrophils, and plasma cells).
12.2 Pharmacodynamics
Adrenal Function in Adults: Four clinical pharmacology studies have been conducted in humans to assess the effect of NASONEX Nasal Spray,
50 mcg at various doses on adrenal function. In one study, daily doses of 200 and 400 mcg of NASONEX Nasal Spray, 50 mcg and 10 mg of prednisone
were compared to placebo in 64 patients (22 to 44 years of age) with allergic rhinitis. Adrenal function before and after 36 consecutive days of treatment
was assessed by measuring plasma cortisol levels following a 6-hour Cortrosyn (ACTH) infusion and by measuring 24-hour urinary free cortisol levels.
NASONEX Nasal Spray, 50 mcg, at both the 200- and 400-mcg dose, was not associated with a statistically significant decrease in mean plasma
cortisol levels post-Cortrosyn infusion or a statistically significant decrease in the 24-hour urinary free cortisol levels compared to placebo. A statistically
significant decrease in the mean plasma cortisol levels post-Cortrosyn infusion and 24-hour urinary free cortisol levels was detected in the prednisone
treatment group compared to placebo.
A second study assessed adrenal response to NASONEX Nasal Spray, 50 mcg (400 and 1600 mcg/day), prednisone (10 mg/day), and placebo,
administered for 29 days in 48 male volunteers (21 to 40 years of age). The 24-hour plasma cortisol area under the curve (AUC
0-24
), during and after an
8-hour Cortrosyn infusion and 24-hour urinary free cortisol levels were determined at baseline and after 29 days of treatment. No statistically significant
differences in adrenal function were observed with NASONEX Nasal Spray, 50 mcg compared to placebo.
A third study evaluated single, rising doses of NASONEX Nasal Spray, 50 mcg (1000, 2000, and 4000 mcg/day), orally administered
mometasone furoate (2000, 4000, and 8000 mcg/day), orally administered dexamethasone (200, 400, and 800 mcg/day), and placebo (administered at
the end of each series of doses) in 24 male volunteers (22 to 39 years of age). Dose administrations were separated by at least 72 hours. Determination
of serial plasma cortisol levels at 8 AM and for the 24-hour period following each treatment were used to calculate the plasma cortisol area under the
curve (AUC
0-24
). In addition, 24-hour urinary free cortisol levels were collected prior to initial treatment administration and during the period immediately
following each dose. No statistically significant decreases in the plasma cortisol AUC, 8 AM cortisol levels, or 24-hour urinary free cortisol levels were
observed in volunteers treated with either NASONEX Nasal Spray, 50 mcg or oral mometasone, as compared with placebo treatment. Conversely,
nearly all volunteers treated with the three doses of dexamethasone demonstrated abnormal 8 AM cortisol levels (defined as a cortisol level <10
mcg/dL), reduced 24-hour plasma AUC values, and decreased 24-hour urinary free cortisol levels, as compared to placebo treatment.
In a fourth study, adrenal function was assessed in 213 patients (18 to 81 years of age) with nasal polyps before and after 4 months of treatment
with either NASONEX Nasal Spray, 50 mcg, (200 mcg once or twice daily) or placebo by measuring 24-hour urinary free cortisol levels. NASONEX
Nasal Spray, 50 mcg, at both doses (200 and 400 mcg/day), was not associated with statistically significant decreases in the 24-hour urinary free cortisol
levels compared to placebo.
Three clinical pharmacology studies have been conducted in pediatric patients to assess the effect of mometasone furoate nasal spray on the
adrenal function at daily doses of 50, 100, and 200 mcg vs. placebo. In one study, adrenal function before and after 7 consecutive days of treatment was
assessed in 48 pediatric patients with allergic rhinitis (ages 6 to 11 years) by measuring morning plasma cortisol and 24-hour urinary free cortisol levels.
Mometasone furoate nasal spray, at all three doses, was not associated with a statistically significant decrease in mean plasma cortisol levels or a
statistically significant decrease in the 24-hour urinary free cortisol levels compared to placebo. In the second study, adrenal function before and after 14
consecutive days of treatment was assessed in 48 pediatric patients (ages 3 to 5 years) with allergic rhinitis by measuring plasma cortisol levels
following a 30-minute Cortrosyn infusion. Mometasone furoate nasal spray, 50 mcg, at all three doses (50, 100, and 200 mcg/day), was not associated
with a statistically significant decrease in mean plasma cortisol levels post-Cortrosyn infusion compared to placebo. All patients had a normal response
to Cortrosyn. In the third study, adrenal function before and after up to 42 consecutive days of once-daily treatment was assessed in 52 patients with
allergic rhinitis (ages 2 to 5 years), 28 of whom received mometasone furoate nasal spray, 50 mcg per nostril (total daily dose 100 mcg), by measuring
morning plasma cortisol and 24-hour urinary free cortisol levels. Mometasone furoate nasal spray was not associated with a statistically significant
decrease in mean plasma cortisol levels or a statistically significant decrease in the 24-hour urinary free cortisol levels compared to placebo.
12.3 Pharmacokinetics
Absorption:
Mometasone furoate monohydrate administered as a nasal spray suspension has very low bioavailability (<1%) in plasma using a sensitive
assay with a lower quantitation limit (LOQ) of 0.25 pcg/mL.
Distribution:
The in vitro protein binding for mometasone furoate was reported to be 98% to 99% in concentration range of 5 to 500 ng/mL.
Metabolism:
Studies have shown that any portion of a mometasone furoate dose which is swallowed and absorbed undergoes extensive metabolism to
multiple metabolites. There are no major metabolites detectable in plasma. Upon in vitro incubation, one of the minor metabolites formed is 6ß-hydroxy-
mometasone furoate. In human liver microsomes, the formation of the metabolite is regulated by cytochrome P-450 3A4 (CYP3A4).
Elimination:
Reference ID: 4281761
This label may not be the latest approved by FDA.
For current labeling information, please visit https://www.fda.gov/drugsatfda
8
Following intravenous administration, the effective plasma elimination half-life of mometasone furoate is 5.8 hours. Any absorbed drug is
excreted as metabolites mostly via the bile, and to a limited extent, into the urine.
Specific Populations:
Hepatic Impairment: Administration of a single inhaled dose of 400 mcg mometasone furoate to subjects with mild (n=4), moderate (n=4), and
severe (n=4) hepatic impairment resulted in only 1 or 2 subjects in each group having detectable peak plasma concentrations of mometasone furoate
(ranging from 50 to 105 pcg/mL). The observed peak plasma concentrations appear to increase with severity of hepatic impairment, however, the
numbers of detectable levels were few.
Renal Impairment: The effects of renal impairment on mometasone furoate pharmacokinetics have not been adequately investigated.
Pediatric: Mometasone furoate pharmacokinetics have not been investigated in the pediatric population [see Use in Specific Populations (8.4)].
Gender: The effects of gender on mometasone furoate pharmacokinetics have not been adequately investigated.
Race: The effects of race on mometasone furoate pharmacokinetics have not been adequately investigated.
Drug-Drug Interactions:
Inhibitors of Cytochrome P450 3A4: In a drug interaction study, an inhaled dose of mometasone furoate 400 mcg was given to 24 healthy
subjects twice daily for 9 days and ketoconazole 200 mg (as well as placebo) were given twice daily concomitantly on Days 4 to 9. Mometasone furoate
plasma concentrations were <150 pcg/mL on Day 3 prior to coadministration of ketoconazole or placebo. Following concomitant administration of
ketoconazole, 4 out of 12 subjects in the ketoconazole treatment group (n=12) had peak plasma concentrations of mometasone furoate >200 pcg/mL on
Day 9 (211-324 pcg/mL).
13 NONCLINICAL TOXICOLOGY
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
In a 2-year carcinogenicity study in Sprague Dawley rats, mometasone furoate demonstrated no statistically significant increase in the incidence
of tumors at inhalation doses up to 67 mcg/kg (approximately 1 and 2 times the maximum recommended daily intranasal dose [MRDID] in adults [400
mcg] and children [100 mcg], respectively, on a mcg/m
2
basis). In a 19-month carcinogenicity study in Swiss CD-1 mice, mometasone furoate
demonstrated no statistically significant increase in the incidence of tumors at inhalation doses up to 160 mcg/kg (approximately 2 times the MRDID in
adults and children, respectively, on a mcg/m
2
basis).
Mometasone furoate increased chromosomal aberrations in an in vitro Chinese hamster ovary-cell assay, but did not increase chromosomal
aberrations in an in vitro Chinese hamster lung cell assay. Mometasone furoate was not mutagenic in the Ames test or mouse-lymphoma assay, and
was not clastogenic in an in vivo mouse micronucleus assay and a rat bone marrow chromosomal aberration assay or a mouse male germ-cell
chromosomal aberration assay. Mometasone furoate also did not induce unscheduled DNA synthesis in vivo in rat hepatocytes.
In reproductive studies in rats, impairment of fertility was not produced by subcutaneous doses up to 15 mcg/kg (less than the MRDID in adults
on a mcg/m
2
basis).
13.2 Animal Toxicology and/or Pharmacology
Reproduction Toxicology Studies
In mice, mometasone furoate caused cleft palate at subcutaneous doses of 60 mcg/kg and above (less than the MRDID in adults on a mcg/m
2
basis). Fetal survival was reduced at 180 mcg/kg (approximately 2 times the MRDID in adults on a mcg/m
2
basis). No toxicity was observed at 20 mcg/kg
(less than the MRDID in adults on a mcg/m
2
basis).
In rats, mometasone furoate produced umbilical hernia at topical dermal doses of 600 mcg/kg and above (approximately 10 times the MRDID in
adults on a mcg/m
2
basis). A dose of 300 mcg/kg (approximately 6 times the MRDID in adults on a mcg/m
2
basis) produced delays in ossification, but no
malformations. In rabbits, mometasone furoate caused multiple malformations (e.g., flexed front paws, gallbladder agenesis, umbilical hernia,
hydrocephaly) at topical dermal doses of 150 mcg/kg and above (approximately 6 times the MRDID in adults on a mcg/m
2
basis). In an oral study,
mometasone furoate increased resorptions and caused cleft palate and/or head malformations (hydrocephaly or domed head) at 700 mcg/kg
(approximately 30 times the MRDID in adults on a mcg/m
2
basis). At 2800 mcg/kg (approximately 110 times the MRDID in adults on a mcg/m
2
basis),
most litters were aborted or resorbed. No toxicity was observed at 140 mcg/kg (approximately 6 times the MRDID in adults on a mcg/m
2
basis).
When rats received subcutaneous doses of mometasone furoate throughout pregnancy or during the later stages of pregnancy, 15 mcg/kg (less
than the MRDID in adults on a mcg/m
2
basis) caused prolonged and difficult labor and reduced the number of live births, birth weight, and early pup
survival. Similar effects were not observed at 7.5 mcg/kg (less than the MRDID in adults on a mcg/m
2
basis).
14 CLINICAL STUDIES
14.1 Allergic Rhinitis in Adults and Adolescents
The efficacy and safety of NASONEX Nasal Spray, 50 mcg in the prophylaxis and treatment of seasonal allergic rhinitis and the treatment of
perennial allergic rhinitis have been evaluated in 18 controlled trials, and one uncontrolled clinical trial, in approximately 3000 adults (ages 17 to 85
years) and adolescents (ages 12 to 16 years). Of the total number of patients, there were 1757 males and 1453 females, including a total of 283
adolescents (182 boys and 101 girls) with seasonal allergic or perennial allergic rhinitis. Patients were treated with NASONEX Nasal Spray 50 mcg at
doses ranging from 50 to 800 mcg/day. The majority of patients were treated with 200 mcg/day. The allergic rhinitis trials evaluated the total nasal
symptom scores that included stuffiness, rhinorrhea, itching, and sneezing. Patients treated with NASONEX Nasal Spray 50 mcg, 200 mcg/day had a
statistically significant decrease in total nasal symptom scores compared to placebo-treated patients. No additional benefit was observed for
mometasone furoate doses greater than 200 mcg/day. A total of 350 patients have been treated with NASONEX Nasal Spray 50 mcg for 1 year or
longer.
In patients with seasonal allergic rhinitis, NASONEX Nasal Spray 50 mcg, demonstrated improvement in nasal symptoms (vs. placebo) within 11
hours after the first dose based on one single-dose, parallel-group study of patients in an outdoor “park” setting (park study) and one environmental
Reference ID: 4281761
This label may not be the latest approved by FDA.
For current labeling information, please visit https://www.fda.gov/drugsatfda
9
exposure unit (EEU) study, and within 2 days in two randomized, double-blind, placebo-controlled, parallel-group seasonal allergic rhinitis studies.
Maximum benefit is usually achieved within 1 to 2 weeks after initiation of dosing.
Prophylaxis of seasonal allergic rhinitis for patients 12 years of age and older with NASONEX Nasal Spray 50 mcg, given at a dose of 200
mcg/day, was evaluated in two clinical studies in 284 patients. These studies were designed such that patients received 4 weeks of prophylaxis with
NASONEX Nasal Spray 50 mcg prior to the anticipated onset of the pollen season; however, some patients received only 2 to 3 weeks of prophylaxis.
Patients receiving 2 to 4 weeks of prophylaxis with NASONEX Nasal Spray 50 mcg demonstrated a statistically significantly smaller mean increase in
total nasal symptom scores with onset of the pollen season as compared to placebo patients.
14.2 Allergic Rhinitis in Pediatrics
The efficacy and safety of NASONEX Nasal Spray 50 mcg in the treatment of seasonal allergic and perennial allergic rhinitis in pediatric patients
(ages 3 to 11 years) have been evaluated in four controlled trials. This included approximately 990 pediatric patients ages 3 to 11 years (606 males and
384 females) with seasonal allergic or perennial allergic rhinitis treated with mometasone furoate nasal spray at doses ranging from 25 to 200 mcg/day.
Pediatric patients treated with NASONEX Nasal Spray 50 mcg (100 mcg total daily dose, 374 patients) had a significant decrease in total nasal symptom
(nasal congestion, rhinorrhea, itching, and sneezing) scores, compared to placebo-treated patients. No additional benefit was observed for the 200-mcg
mometasone furoate total daily dose in pediatric patients (ages 3 to 11 years). A total of 163 pediatric patients have been treated for 1 year.
14.3 Nasal Polyps in Adults 18 Years of Age and Older
Two studies were performed to evaluate the efficacy and safety of NASONEX Nasal Spray in the treatment of nasal polyps. These studies
involved 664 patients with nasal polyps, 441 of whom received NASONEX Nasal Spray. These studies were randomized, double-blind, placebo-
controlled, parallel-group, multicenter studies in patients 18 to 86 years of age with bilateral nasal polyps. Patients were randomized to receive
NASONEX Nasal Spray 200 mcg once daily, 200 mcg twice daily or placebo for a period of 4 months. The co-primary efficacy endpoints were 1) change
from baseline in nasal congestion/obstruction averaged over the first month of treatment; and 2) change from baseline to last assessment in bilateral
polyp grade during the entire 4 months of treatment as assessed by endoscopy. Efficacy was demonstrated in both studies at a dose of 200 mcg twice
daily and in one study at a dose of 200 mcg once a day (see TABLE 2 below).
TABLE 2: EFFECT OF NASONEX NASAL SPRAY IN TWO RANDOMIZED, PLACEBO-CONTROLLED TRIALS IN PATIENTS WITH NASAL
POLYPS
NASONEX
200 mcg qd
NASONEX
200 mcg bid
Placebo
P-value for
NASONEX
200 mcg qd vs.
placebo
P-value for
NASONEX
200 mcg bid vs.
placebo
Study 1
N=115
N=122
N=117
Baseline bilateral polyp grade*
4.21
4.27
4.25
Mean change from baseline in bilateral polyps grade
-1.15
-0.96
-0.50
<0.001
0.01
Baseline nasal congestion
†
2.29
2.35
2.28
Mean change from baseline in nasal congestion
-0.47
-0.61
-0.24
0.001
<0.001
Study 2
N=102
N=102
N=106
Baseline bilateral polyp grade*
4.00
4.10
4.17
Mean change from baseline in bilateral polyps grade
-0.78
-0.96
-0.62
0.33
0.04
Baseline nasal congestion
†
2.23
2.20
2.18
Mean change from baseline in nasal congestion
-0.42
-0.66
-0.23
0.01
<0.001
* polyps in each nasal fossa were graded by the investigator based on endoscopic visualization, using a scale of 0-3 where 0=no polyps; 1=polyps in the
middle meatus, not reaching below the inferior border of the middle turbinate; 2=polyps reaching below the inferior border of the middle turbinate but not
the inferior border of the inferior turbinate; 3=polyps reaching to or below the border of the inferior turbinate, or polyps medial to the middle turbinate
(score reflects sum of left and right nasal fossa grades).
†
nasal congestion/obstruction was scored daily by the patient using a 0-3 categorical scale where 0=no symptoms, 1=mild symptoms, 2=moderate
symptoms and 3=severe symptoms.
There were no clinically relevant differences in the effectiveness of NASONEX Nasal Spray, 50 mcg, in the studies evaluating treatment of nasal
polyps across subgroups of patients defined by gender, age, or race.
14.4 Nasal Congestion Associated with Seasonal Allergic Rhinitis
The efficacy and safety of NASONEX Nasal Spray 50 mcg for nasal congestion associated with seasonal allergic rhinitis were evaluated in three
randomized, placebo-controlled, double blind clinical trials of 15 days duration. The three trials included a total of 1008 patients 12 years of age and
older with nasal congestion associated with seasonal allergic rhinitis, of whom 506 received NASONEX Nasal Spray 200 mcg daily and 502 received
placebo. Of the 1008 patients, the majority 784 (78 %) were Caucasians. The majority of the patients were between 18 to < 65 years of age with a mean
age of 38.8 years and were predominantly women (66%). The primary efficacy endpoint was the change from baseline in average morning and evening
reflective nasal congestion score over treatment day 1 to day 15. The key secondary efficacy endpoint was the change from baseline in average
morning and evening reflective total nasal symptom score (TNSS=rhinorrhea [nasal discharge/runny nose or postnasal drip], nasal
congestion/stuffiness, nasal itching, sneezing) averaged over treatment day 1 to 15. Two out of three studies demonstrated that treatment with
NASONEX Nasal Spray significantly reduced the nasal congestion symptom score and the TNSS compared to placebo in patients 12 years of age and
older with seasonal allergic rhinitis (see TABLE 3 and 4 below).
Reference ID: 4281761
This label may not be the latest approved by FDA.
For current labeling information, please visit https://www.fda.gov/drugsatfda
10
TABLE 3: EFFECT OF NASONEX NASAL SPRAY IN TWO RANDOMIZED, PLACEBO-CONTROLLED TRIALS ON NASAL CONGESTION IN
PATIENTS WITH SEASONAL ALLERGIC RHINITIS
Treatment (Patient Number)
Baseline *
LS Mean
†
Change from Baseline
LS Mean
†
Difference from
Placebo
LS Mean
†
P-value for
NASONEX 200 mcg qd
vs. placebo
Study 1
NASONEX 200 mcg qd (N=176)
2.63
-0.64
-0.15
0.006
Placebo (N=175)
2.62
-0.49
Study 2
NASONEX 200 mcg qd (N=168)
2.62
-0.71
-0.31
<0.001
Placebo (N=164)
2.60
-0.40
* nasal congestion/obstruction was scored daily by the patient using a 0-3 categorical scale where 0=no symptoms, 1=mild symptoms, 2=moderate
symptoms and 3=severe symptoms.
†
LS Mean and p-value was from an ANCOVA model with treatment, baseline value, and center effects.
TABLE 4: EFFECT OF NASONEX NASAL SPRAY ON TNSS IN TWO RANDOMIZED, PLACEBO-CONTROLLED TRIALS IN PATIENTS WITH
SEASONAL ALLERGIC RHINITIS
Treatment (Patient Number)
Baseline *
LS Mean
†
Change from Baseline
LS Mean
†
Difference from
Placebo
LS Mean
†
P-value for
NASONEX 200 mcg qd
vs. placebo
Study 1
NASONEX 200 mcg qd (N=176)
9.60
-2.68
-0.83
<0.001
Placebo (N=175)
9.66
-1.85
Study 2
NASONEX 200 mcg qd (N=168)
9.39
-3.00
-1.27
<0.001
Placebo (N=164)
9.50
-1.73
* TNSS was the sum of four individual symptom scores: rhinorrhea, nasal congestion/stuffiness, nasal itching and sneezing. Each symptom was to be
rated on a scale of 0=none, 1=mild, 2=moderate, 3=severe.
†
LS Mean and p-value was from an ANCOVA model with treatment, baseline value, and center effects.
Based on results in other studies with NASONEX Nasal Spray in pediatric patients, effects on nasal congestion associated with seasonal allergic
rhinitis in patients below 12 years of age is similar to those seen in adults and adolescents [see Clinical Studies (14.2)].
16 HOW SUPPLIED/STORAGE AND HANDLING
NASONEX (mometasone furoate monohydrate) Nasal Spray, 50 mcg is supplied in a white, high-density, polyethylene bottle fitted with a white
metered-dose, manual spray pump, and blue cap. It contains 17 g of product formulation, 120 sprays, each delivering 50 mcg of mometasone furoate
per actuation.
(NDC 0085-1288-01).
Store at 25°C (77°F); excursions permitted to 15-30°C (59-86°F) [see USP Controlled Room Temperature]. Protect from light.
When NASONEX Nasal Spray, 50 mcg is removed from its cardboard container, prolonged exposure of the product to direct light
should be avoided. Brief exposure to light, as with normal use, is acceptable.
SHAKE WELL BEFORE EACH USE.
Keep out of reach of children.
17 PATIENT COUNSELING INFORMATION
Advise the patient to read the FDA-approved patient labeling (Patient Information).
17.1 Local Nasal Effect
Patients should be informed that treatment with NASONEX Nasal Spray 50 mcg may be associated with adverse reactions which include
epistaxis (nose bleed) and nasal septum perforation. Candida infection may also occur. Because of the inhibitory effect of corticosteroids on wound
Reference ID: 4281761
This label may not be the latest approved by FDA.
For current labeling information, please visit https://www.fda.gov/drugsatfda

11
healing, patients who have experienced recent nasal septum ulcers, nasal surgery, or nasal trauma should not use a nasal corticosteroid until healing
has occurred [see Warnings and Precautions (5.1)]. Patients should be cautioned not to spray NASONEX Nasal Spray 50 mcg directly onto the nasal
septum.
17.2 Glaucoma and Cataracts
Advise patients that long-term use of nasal and inhaled corticosteroids may increase the risk of some eye problems (glaucoma or cataracts);
regular eye examinations should be considered. Patients should be cautioned not to spray NASONEX Nasal Spray 50 mcg into the eyes [see Warnings
and Precautions (5.2)].
17.3 Immunosuppression
Persons who are on immunosuppressant doses of corticosteroids should be warned to avoid exposure to chickenpox or measles, and patients
should also be advised that if they are exposed, medical advice should be sought without delay [see Warnings and Precautions (5.4)].
17.4 Use Regularly for Best Effect
Patients should use NASONEX Nasal Spray 50 mcg on a regular basis for optimal effect. Improvement in nasal symptoms of allergic rhinitis has
been shown to occur within 1 to 2 days after initiation of dosing. Maximum benefit is usually achieved within 1 to 2 weeks after initiation of dosing.
Patients should not increase the prescribed dosage but should contact their physician if symptoms do not improve, or if the condition worsens.
Administration to young children should be aided by an adult.
If a patient missed a dose, the patient should be advised to take the dose as soon as they remember. The patient should not take more than the
recommended dose for the day.
Manufactured by: MSD International GmbH (Singapore Branch), Singapore 638414, Singapore
For patent information: www.merck.com/product/patent/home.html
Copyright © 1997-XXXX Merck Sharp & Dohme Corp., a subsidiary of Merck & Co., Inc.
All rights reserved.
uspi-mk0887-ns-xxxxrxxx
Reference ID: 4281761
This label may not be the latest approved by FDA.
For current labeling information, please visit https://www.fda.gov/drugsatfda

1
PATIENT INFORMATION
NASONEX® [nā-zə-neks] 50 mcg
(mometasone furoate monohydrate)
Nasal Spray
For Intranasal Use Only
Read the Patient Information that comes with NASONEX before you start using it and each time you get a refill. There may be
new information. This Patient Information does not take the place of talking to your healthcare provider about your medical
condition or treatment. If you have any questions about NASONEX, ask your healthcare provider.
What is NASONEX?
NASONEX Nasal Spray is a man-made (synthetic) corticosteroid medicine that is used to:
• treat the nasal symptoms of seasonal and year-round allergic rhinitis (inflammation of the lining of the nose) in adults and
children 2 years of age and older.
• treat nasal congestion that happens with seasonal allergic rhinitis in adults and children 2 years of age and older.
• prevent nasal symptoms of seasonal allergic rhinitis in people 12 years of age and older.
• treat nasal polyps in people 18 years and older.
• It is not known if NASONEX Nasal Spray is safe and effective in children under:
• 2 years of age to treat allergic rhinitis.
• 18 years of age to treat nasal polyps.
Who should not use NASONEX?
Do not use NASONEX if you are allergic to mometasone furoate or any of the ingredients in NASONEX. See the end of this
leaflet for a complete list of ingredients in NASONEX.
What should I tell my healthcare provider before and during treatment with NASONEX?
Before you take NASONEX, tell your healthcare provider about all of your medical conditions, including if you:
• have had recent nasal sores, nasal surgery, or nasal injury.
• have eye or vision problems, such as cataracts, glaucoma (increased pressure in your eye), and blurred vision, or other
changes in your vision.
• have tuberculosis or any untreated fungal, bacterial, viral infections, or eye infections caused by herpes.
• have been near someone who has chickenpox or measles.
• are not feeling well or have any other symptoms that you do not understand.
• are pregnant or planning to become pregnant. It is not known if NASONEX will harm your unborn baby. Talk to your
healthcare provider if you are pregnant or plan to become pregnant.
• are breastfeeding or planning to breastfeed. It is not known whether NASONEX passes into your breast milk.
Tell your healthcare provider about all the medicines you take including prescription and over-the-counter medicines,
vitamins, and herbal supplements.
Especially tell your healthcare provider if you take:
• certain medicines for HIV (such as ritonavir, atazanavir, indinavir, nelfinavir, and saquinavir)
• cobicistat-containing products
• certain antifungals (such as ketoconazole and itraconazole)
• certain antibiotics (such as clarithromycin and telithromycin)
• certain antidepressants (such as nefazodone)
If you take these medicines with NASONEX, your healthcare provider should monitor you for side effects.
NASONEX may affect the way other medicines work, and other medicines may affect how NASONEX works.
Know the medicines you take. Keep a list of them to show your healthcare provider and pharmacist when you get a new
medicine.
How should I use NASONEX?
• Use NASONEX exactly as prescribed by your healthcare provider.
• This medicine is for use in the nose only. Do not spray it into your mouth or eyes.
• An adult should help a young child use this medicine.
• For best results, you should keep using NASONEX regularly each day without missing a dose. If you do miss a dose of
NASONEX, take it as soon as you remember. However, do not take more than the daily dose prescribed by your healthcare
provider.
• Do not use NASONEX more often than prescribed. Ask your healthcare provider if you have any questions.
• For detailed instructions on how to use NASONEX Nasal Spray, see the “Patient Instructions for Use” at the end of this
Reference ID: 4281761
This label may not be the latest approved by FDA.
For current labeling information, please visit https://www.fda.gov/drugsatfda

2
leaflet.
• See your healthcare provider regularly to check your symptoms while taking NASONEX and to check for side effects.
What should I avoid while taking NASONEX?
If you are taking other corticosteroid medicines for allergy, by mouth or injection, your healthcare provider may advise you to
stop taking them after you begin using NASONEX.
What are the possible side effects of NASONEX?
NASONEX may cause serious side effects, including:
• thrush (candida), a fungal infection in your nose and throat. Tell your healthcare provider if you have any redness or
white colored patches in your nose or throat.
• hole in the cartilage of the nose (nasal septal perforation). A whistling sound when you breathe may be a symptom of
nasal septum perforation.
• slow wound healing. Do not use NASONEX until your nose has healed if you have a sore in your nose, if you have surgery
on your nose, or if your nose has been injured.
• eye problems, including glaucoma, cataracts, and blurred vision. You should have regular eye exams.
• allergic reactions. Allergic reactions including wheezing may happen after using NASONEX. If wheezing happens stop using
NASONEX. Tell your healthcare provider or get medical help right away.
• immune system problems that may increase your risk of infections. You are more likely to get infections if you take
medicines that weaken your immune system. Avoid contact with people who have contagious diseases such as chicken pox
or measles while using NASONEX. Symptoms of infection may include: fever, pain, aches, chills, feeling tired, nausea, and
vomiting. Tell your healthcare provider about any signs of infection while you are using NASONEX.
• adrenal insufficiency. Adrenal insufficiency is a condition in which the adrenal glands do not make enough steroid
hormones. Symptoms of adrenal insufficiency can include: tiredness, weakness, nausea and vomiting, and low blood
pressure.
• slowed growth in children. Your child’s growth should be checked regularly while using NASONEX.
The most common side effects of NASONEX include:
• headache
• viral infection
• sore throat
• nosebleeds
• cough
These are not all the possible side effects of NASONEX. Call your healthcare provider for medical advice about side effects.
You may report side effects to FDA at 1-800-FDA-1088.
How should I store NASONEX?
• Store NASONEX at room temperature between 59°F to 86°F (15°C to 30°C).
• Protect from light.
• Avoid prolonged exposure of NASONEX container to direct light.
• Shake well before each use.
• Keep NASONEX and all medicines out of the reach of children.
General information about the safe and effective use of NASONEX.
Medicines are sometimes prescribed for conditions that are not listed in a Patient Information leaflet. Do not use NASONEX for
a condition for which it was not prescribed. Do not give NASONEX to other people even if they have the same symptoms you
have. It may harm them.
You can ask your healthcare provider or pharmacist for information about NASONEX that is written for health professionals.
What are the ingredients in NASONEX?
Active ingredient: mometasone furoate monohydrate
Inactive ingredients: glycerin, microcrystalline cellulose and carboxymethylcellulose sodium, sodium citrate, citric acid,
benzalkonium chloride, and polysorbate 80.
For more information, go to www.NASONEX.com or call 1-800-622-4477.
This Patient Information has been approved by the U.S. Food and Drug Administration Revised: 06/2018
Reference ID: 4281761
This label may not be the latest approved by FDA.
For current labeling information, please visit https://www.fda.gov/drugsatfda
3
Patient Instructions for Use
For use in your nose only.
Read the Patient Instructions for Use carefully before you start to use your NASONEX Nasal Spray. If you have any
questions, ask your healthcare provider.
Shake the bottle well before each use.
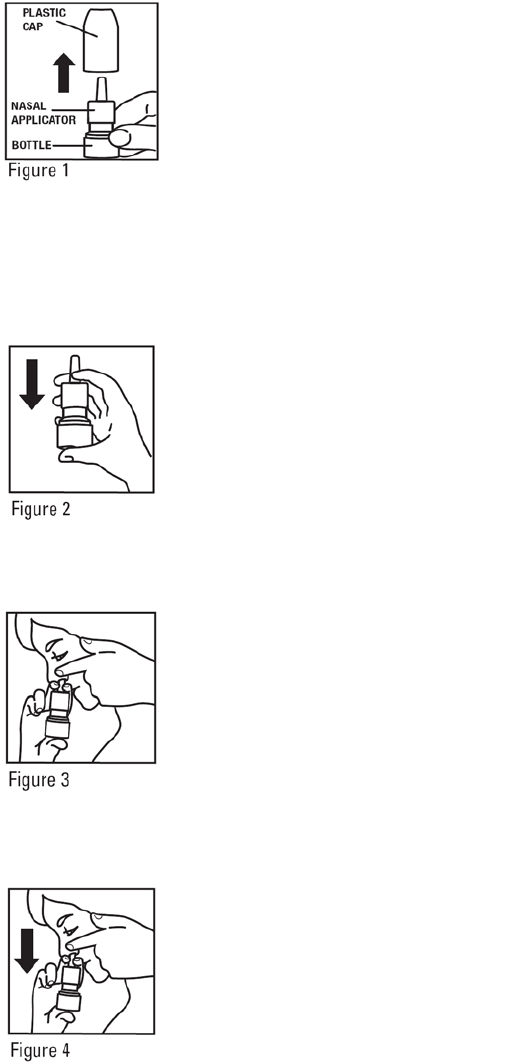
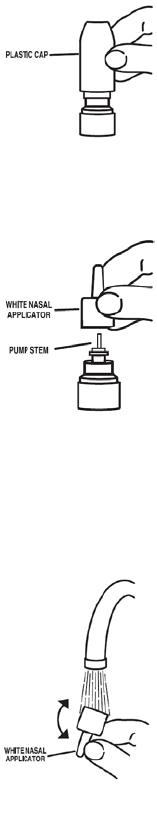
1. Remove the plastic cap (See Figure 1).
2. Before you use NASONEX for the first time, prime the pump by pressing downward on the shoulders of the white nasal
applicator using your index finger and middle finger while holding the base of the bottle with your thumb (See Figure 2).
Do Not pierce the nasal applicator. Press down and release the pump 10 times or until a fine spray appears. Do Not
spray into eyes. The pump is now ready to use. The pump may be stored unused for up to 1 week without repriming. If
unused for more than 1 week, reprime by spraying 2 times or until a fine spray appears.
3. Gently blow your nose to clear the nostrils. Close 1 nostril. Tilt your head forward slightly, keep the bottle upright,
carefully insert the nasal applicator into the other nostril (See Figure 3). Do Not spray directly onto the nasal septum (the
wall between the two nostrils).
4. For each spray, hold the spray bottle upright and press firmly downward 1 time on the shoulders of the white nasal
applicator using your index and middle fingers while supporting the base of the bottle with your thumb. Breathe gently
inward through the nostril (See Figure 4).
5. Then breathe out through the mouth.
Note: It is important to keep the NASONEX
unit in an upright orientation (as seen in
Figure 4). Failure to do so may result in an
incomplete or non-existent spray.
Reference ID: 4281761
This label may not be the latest approved by FDA.
For current labeling information, please visit https://www.fda.gov/drugsatfda
4
6. Repeat in the other nostril.
7. Wipe the nasal applicator with a clean tissue and replace the plastic cap.
Each bottle of NASONEX Nasal Spray contains enough medicine for you to spray medicine from the bottle 120 times. Do not
use the bottle of NASONEX Nasal Spray after 120 sprays. Additional sprays after the 120 sprays may not contain the right
amount of medicine, you should keep track of the number of sprays used from each bottle of NASONEX Nasal Spray, and
throw away the bottle even if it has medicine still left in. Do not count any sprays used for priming the device. Talk with your
healthcare provider before your supply runs out to see if you should get a refill of your medicine.
Pediatric Use: Administration to young children should be done by an adult. Steps 1 through 7 from the Patient Instructions
for Use, should be followed.
Cleaning: Do not try to unblock the nasal applicator with a sharp object. Please see Patient Instructions for Cleaning
Applicator.
Patient Instructions for Cleaning Applicator
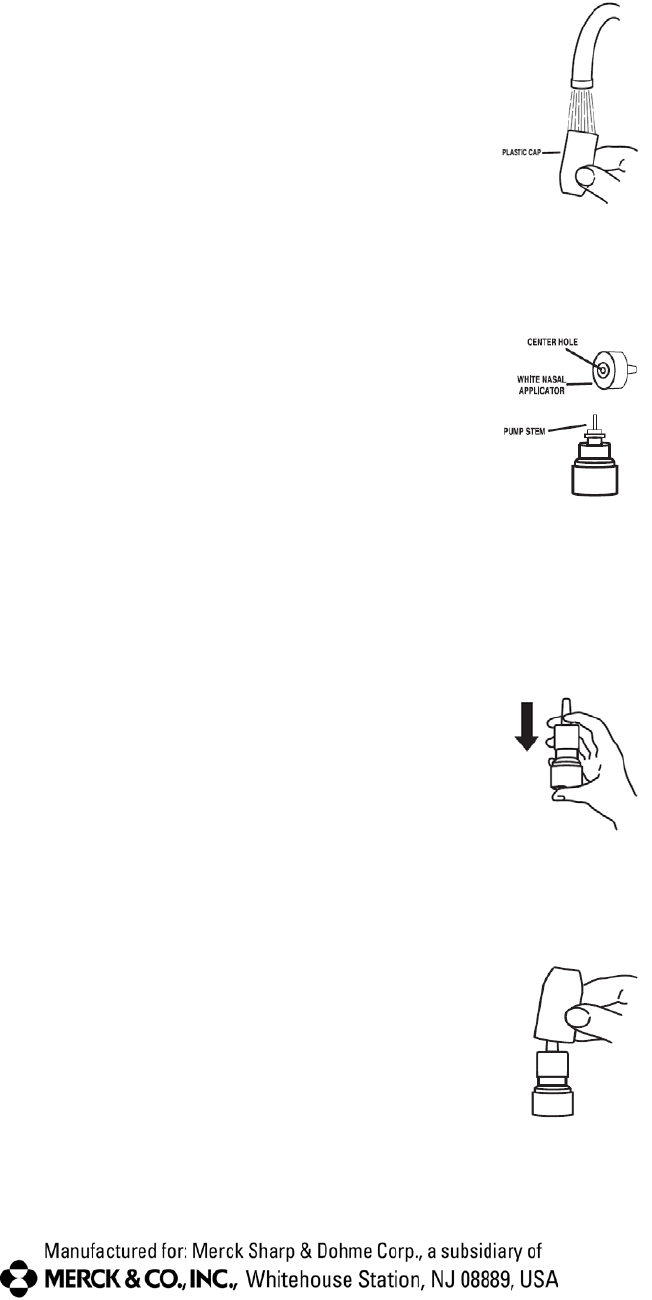
1. To clean the nasal applicator, remove the plastic cap (See Figure 5).
2. Pull gently upward on the white nasal applicator to remove (See Figure 6).
3. Soak the nasal applicator in cold tap water and rinse both ends of the nasal applicator under cold tap water and dry (See
Figure 7). Do not try to unblock the nasal applicator by inserting a pin or other sharp object as this will damage
the applicator and cause you not to get the right dose of medicine.
4. Rinse the plastic cap under cold water and dry (See Figure 8).
Figure 5
Figure 6
Figure 7
Reference ID: 4281761
This label may not be the latest approved by FDA.
For current labeling information, please visit https://www.fda.gov/drugsatfda
5
5. Put the nasal applicator back together making sure the pump stem is reinserted into the applicator’s center hole (See
Figure 9).
6. Reprime the pump by pressing downward on the shoulders of the white nasal applicator using your index and middle
fingers while holding the base of the bottle with your thumb. Press down and release the pump 2 times or until a fine
spray appears. Do Not spray into eyes. The pump is now ready to use. The pump may be stored unused for up to 1
week without repriming. If unused for more than 1 week, reprime by spraying 2 times or until a fine spray appears (See
Figure 10).
7. Replace the plastic cap (See Figure 11).
Manufactured by: MSD International GmbH (Singapore Branch), Singapore 638414, Singapore
For patent information: www.merck.com/product/patent/home.html
Copyright © 1997-XXXX Merck Sharp & Dohme Corp., a subsidiary of Merck & Co., Inc.
Figure 8
Figure 9
Figure 10
Figure 11
Reference ID: 4281761
This label may not be the latest approved by FDA.
For current labeling information, please visit https://www.fda.gov/drugsatfda
6
All rights reserved.
This Patient Information and Instructions for Use has been approved by the U.S. Food and Drug Administration.
Revised: 06/2018
usppi-mk0887-ns-xxxxrxxx
Reference ID: 4281761
This label may not be the latest approved by FDA.
For current labeling information, please visit https://www.fda.gov/drugsatfda
